The $77 Billion Efficiency
The Economic Case for Longitudinal Data
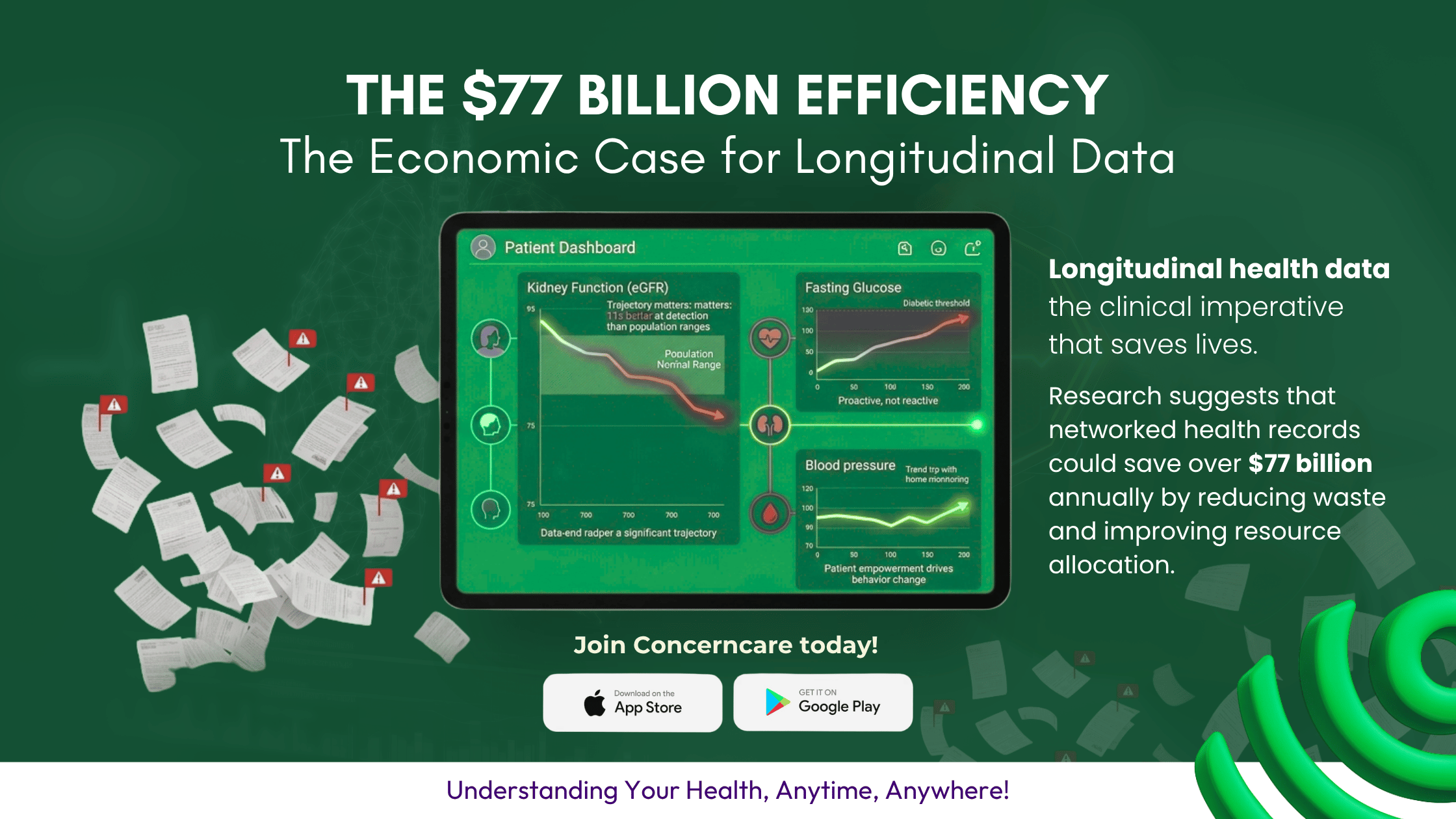
The $77 Billion Efficiency
In the global discourse on healthcare reform, the conversation frequently centers on the high cost of new pharmaceuticals or advanced surgical robotics. However, a far more significant economic lever remains largely untapped: the efficiency of our medical information systems. The persistence of fragmented, paper-based, or siloed digital records is not just a clinical failure; it is a profound economic drain.
A growing body of economic research suggests that the widespread adoption of networked, longitudinal health records could save global healthcare systems over $77 billion annually by eliminating systemic waste and optimizing resource allocation.
The Anatomy of Healthcare Waste
Healthcare spending is increasingly dominated by "administrative complexity" and "clinical inefficiency" terms that describe the friction of moving a patient through a system that does not remember them. In the United States alone, waste is estimated to reach $1.6 trillion annually as of 2026, with administrative costs and fragmented care coordination accounting for a significant portion of this figure.
The economic "backfalls" of fragmented data manifest in three primary ways:
- Redundant Diagnostic Testing: When a patient is referred to a specialist or visits an emergency department without their prior records, clinicians frequently order new blood tests and imaging to ensure safety. It is estimated that up to 20% of all medical tests are redundant, performed simply because the previous results were inaccessible.
- Medical Error and Liability: Diagnostic errors often driven by missing information are a primary driver of malpractice claims. Reducing these errors through longitudinal history tracking doesn't just save lives; it stabilizes insurance premiums and reduces the billions spent on legal defense and settlements.
- Inefficient Care Transitions: Every time a patient moves between facilities, the lack of data interoperability requires manual data entry and phone-based verification. This "interoperability maze" costs the healthcare system billions in lost productivity for clinicians and administrative staff.
The Return on Investment (ROI) of Longitudinal Data
The transition to advanced, longitudinal electronic health records (EHRs) is a capital-intensive process, but the long-term ROI is undeniable. A 2026 national sample analysis revealed that patients treated in hospitals with advanced, integrated EHRs cost, on average, 9.66% less per admission than those in hospitals with fragmented systems.
The economic case is even stronger for chronic disease management. Managing a patient with multiple co-morbidities such as diabetes and hypertension requires a continuous "thread" of data to prevent expensive acute crises. By identifying a declining trend in kidney function or a rising HbA1c months before it leads to a hospital admission, longitudinal systems shift the economic burden from high-cost emergency care to low-cost preventive management.
Sub-Saharan Africa: The Opportunity of Leapfrogging
For emerging markets in Sub-Saharan Africa, the economic stakes are even higher. These systems are currently at a crossroads: they can continue to build on fragmented paper silos, or they can "leapfrog" directly into unified, longitudinal digital systems like ConcernCare.
The economic benefit in this region is two-fold. First, it maximizes the impact of limited healthcare budgets by ensuring that every dollar spent on a diagnostic test is "saved" in a permanent digital record. Second, it creates an environment of informational transparency that is attractive to international health payers and investors. When healthcare outcomes can be verified with longitudinal data, the entire system becomes more bankable and sustainable.
Strategic Implementation: The Path Forward
To capture the $77 billion efficiency, healthcare leaders must move beyond the "snapshot" model of data collection. Strategic investment should be directed toward:
- Interoperable Infrastructure: Ensuring that data follows the patient across different providers and facilities.
- Patient-Centered Portability: Empowering patients to carry their own "health story" in a secure, digital format.
- Predictive Analytics: Utilizing the temporal dimension of longitudinal data to identify high-risk, high-cost patients before they reach a crisis point.
Final Thought
The "77 Billion Efficiency" is not a theoretical projection; it is a target that is achievable with current technology. By treating medical data as a continuous asset rather than a series of isolated events, we can build a healthcare economy that is more resilient, more equitable, and fundamentally more efficient. The most valuable currency in 2026 is not just the data itself, but the continuity of that data over time.
Download ConcernCare
Fresh Perspectives, Timeless Wisdom Explore Our Latest Blog Edition
View AllJoin our newsletter to stay up to date on features and releases
Stay in the loop with exclusive updates, sneak peeks, and insider tips that will elevate your experience. Don’t miss out


